The various techniques for breast reconstruction
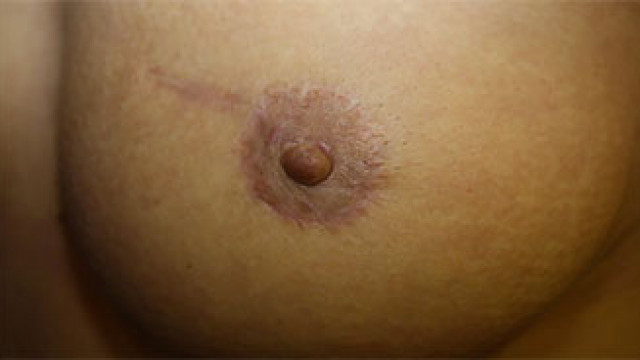
Several techniques are possible. The one most satisfaying to me is the use of a skin graft withdrawn from the genital region for areola reconstruction, associated when possible to the opposite nipple graft after bipartition ( if there is enough volume). This technique has great results and leaves no sequels in the genital area. It causes no pain nor alteration of the sensivity to the nipple withdrawn. The areola coloration after a few weeks is the same as the opposite areola. If the coloration starts to fade with years, an additional tattoo can be done. That way, the result will look a lot more natural than a sole reconstruction with tattoo. If the opposite nipple is too small, nipple reconstruction can be carried out with a local skin flap that will necessarily be quite small for reconstructions with prosthesis, given the limited thickness available. Others breast reconstruction techniques
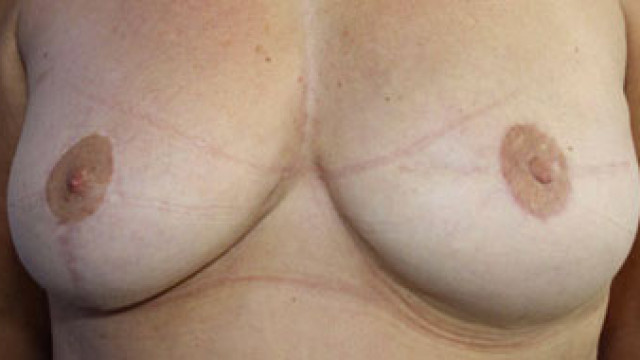
Lipofilling is the injection of the patient’s own fat tissue, withdrawn through liposuction, then purified by centrifugation and reinjected during the same operation. ( This injection is done as a graft of fat cellular tissue using a thin needle, in a retrograde manner, over several plans, and crosswise. The volume that can be injected is limited by the thickness of the injected area. Several sessions are often necessary. This technique that seems simple, actually requires as ignificant learning curvein order to inject properly and avoid the formation ofoily cysts. Lipofillingis used very frequently inbreast reconstruction,associated with other reconstructions or sometimes by itself.Its only limit is the lack of fat sampling area. The percentage of fat resorption after injection is between 30 and50%, and higher for smoking patients. This technique changed completely the results of breast reconstruction with prosthesis. Despite the very important choice that we currently have in breast prosthesis, there are no custom-made prostheses. As one of my Brazilian colleagues likes to say, lipofilling is somehow the « Photoshop » of breast reconstruction. In some cases, it can correct the volume of the reconstructed breast. It is very useful to improve the contours of the reconstruction. In other situations, it […]
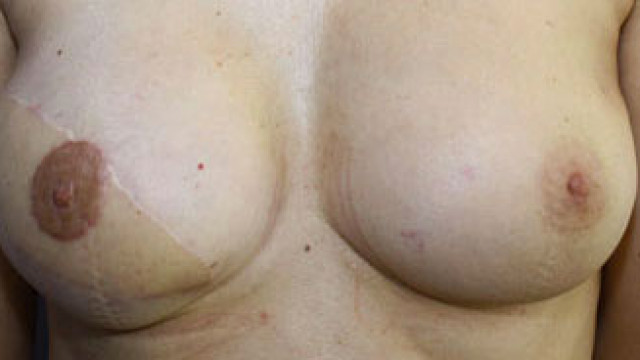
The dorsal flap (latissimus dorsi) is technically simpler to carry out than the TRAM. The vascularization is safer than with an abdominal flap and can be offered to patients for who a TRAM is not suitable due to a vascular problem or smoking habits. It experienced a great development in recent years thanks to an increase in possible secondary volume using lipofilling, which permits to realize autologous dorsal flaps. It has the disadvantage of associating a dorsal scar and the volume obtained is more limited than with a TRAM. The follow-up after surgery is easier than the TRAM’s and a full recovery is expected within 6 weeks. In my practice, I use it as an autologous graft for breasts of small or average volume and more rarely for bigger volumes. I add a prosthesis behind the flap if a substantial volume is necessary. In that case, the progressive risk (capsula contracture and asymmetry over time) is the same as a reconstruction with prosthesis. Reconstruction techniques
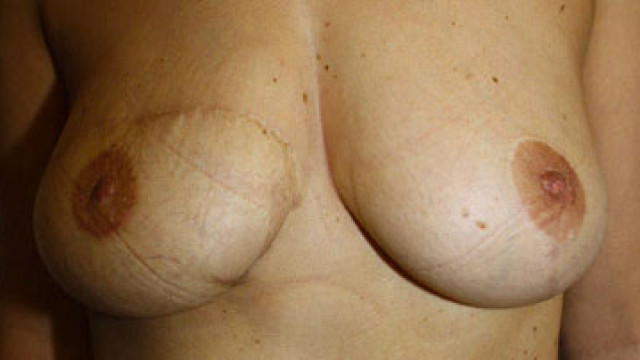
This is a technique I have extensive experience of (with over 600 TRAMs carried out since 1989), and for which I have set up a procedure making it very reliable, reducing to 1% the risk of partial flap necrosis. The TRAM is a flap using one of the two rectal muscles from the abdominal wall, sectioned on its lower part, in which circulate epigastric vessels that allow blood circulation in the fat and skin flap. Superior and inferior epigastric vessels all meet in the rectus abdominal muscle. Before preparation, inferior epigastric vascular flow is predominant. To improve vascular blood flow (and thus reduce the risk of a poor vascularization and a subsequent flap necrosis) a preparation has to be done beforehand. It consists in a ligation of the inferior epigastric vessels, which reverts the impulse of the vascular blood flow and permits the resumption of vascularization for inferior epigastric vessels It can be done through surgery (sometimes in the same time as the mastectomy, if this reconstruction is planned from the start) or through embolization (at the vascular radiology department of the Clinique de l’Orangerie, under local anesthesia). The angiography scan made subsequently shows the quality of the superior epigastric […]
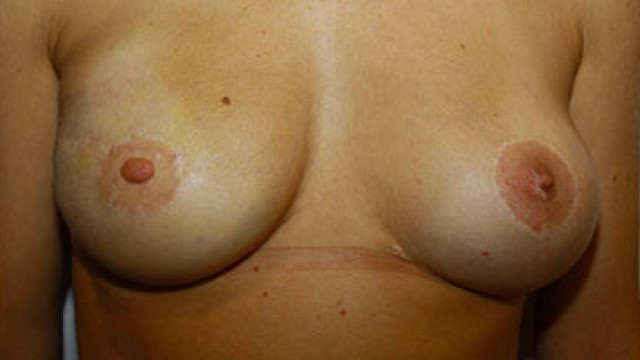
It can be realized immediately or secondarily. I usually use a tissue expander, placed in sub muscular position, that will be swollen post-operatively every 3 to 4 weeks with saline solution. The expander will be changed within 4 to 12 months to a final silicone prosthesis. This techniques enables the patient to choose the volume as the expansion takes place. The use of an expander in immediate reconstruction diminishes scar tension and the risk of complications. In secondary reconstruction, the expander enables to get a well-marked mammary fold without having to perform a skin and fat flap advancement and the risks that it involves. In my experience,the risk of failureof breast reconstruction with prosthesis using anexpanderis low (3%), compared to the riskof complicationsafter introduction of apermanent prosthesisimmediately, (5 to20%according to literature), especially for patients who smoke. The inconvenience of having to carry out a second operation is not only compensated by a lower risk, but also by the opportunity to obtain a better final result: -by using anatomic implants when replacing the expander, giving out a more natural curve than round prostheses – remodeling easily the space for the prosthesis, if the height of the fold or the implant’s width needs […]

 English
English
 Français
Français
 中文 (中国)
中文 (中国)
 Español
Español
 Português (BR)
Português (BR)